Walk into any pharmacy and the probiotic shelf has the confident energy of a section that has already won the argument. Dozens of products, billions of CFUs, strain names that sound like pharmaceutical compounds. The implicit promise is consistent: swallow these, fix your gut.
The evidence tells a more complicated story.
The Claim: Beneficial Bacteria, Delivered Daily
The logic behind probiotics is genuinely not crazy. Your gut microbiome — trillions of bacteria, fungi, and other microorganisms — is implicated in digestion, immune function, mood, and more. If certain bacterial profiles are associated with better health outcomes, why not supplement the good ones directly?
This reasoning, combined with savvy marketing and a cultural moment around "gut health," has built a multibillion-dollar industry. The assumption embedded in most probiotic products is that swallowing live microorganisms will meaningfully alter your microbiome's composition for the better.
The Appeal: A Tractable Problem in an Intractable Body
Part of what makes probiotics so appealing is that they offer agency. The gut microbiome feels important and mysterious; a capsule feels like a concrete response to that mystery. The wellness industry has been extraordinarily good at channeling legitimate scientific excitement — microbiome research genuinely exploded in the early 2000s — into product categories that outrun the actual evidence.
There's also a plausibility halo. Fermented foods have been part of human diets for millennia. Yogurt, kimchi, kefir — these feel like food, not medicine, which lowers skepticism. If grandma's yogurt was good for her gut, surely a concentrated capsule version is even better.
The Evidence: Strain-Specific, Population-Specific, and Frequently Inconclusive
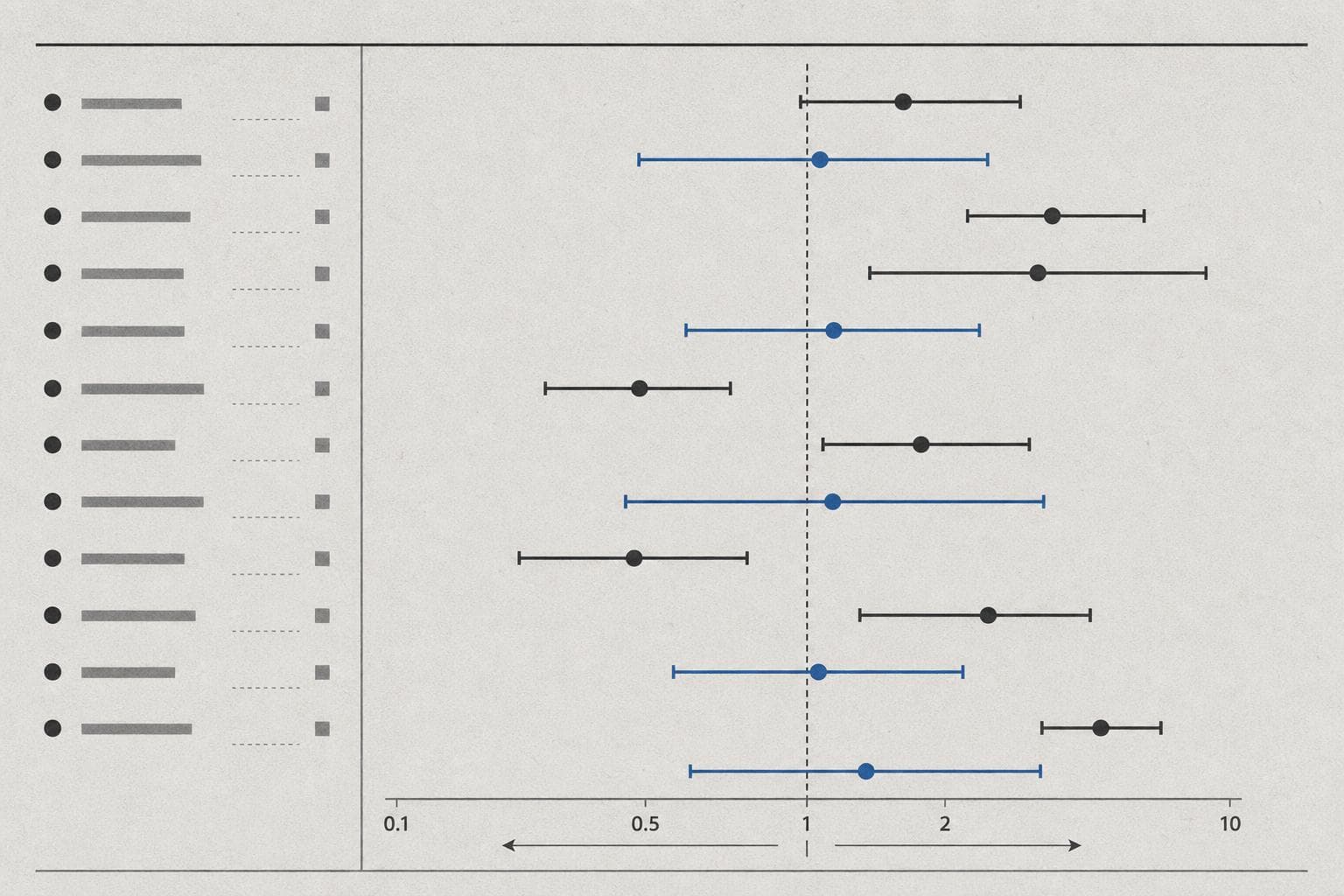
Here's where the story gets uncomfortable for the industry. As a gastroenterologist writing in Oprah Daily put it bluntly: more than 1,000 clinical trials of probiotics have been conducted, and the research is "all over the map — different bacterial strains, different doses, wildly different outcomes being measured." Even meta-analyses, which are supposed to synthesize messy individual studies into cleaner signals, "refuse to tell a coherent story."
The NIH's health professional fact sheet on probiotics reflects the same picture: evidence exists for specific strains in specific conditions, but generalizing across strains or populations is not supported. The FDA does not consider over-the-counter probiotics to be drugs — meaning they don't require the same evidence of efficacy before hitting shelves.
The most interesting recent research suggests why the clinical trials are so messy. A 2026 study published in Nature Communications analyzed over 51,000 gut microbiomes across 149 cohorts and found that whether a probiotic strain actually colonizes and persists in your gut depends heavily on your baseline microbiome composition. The researchers developed what they call "Receptive Scores" — a measure of how permissive a given person's existing microbiome is to a particular Bifidobacterium strain. Across eight probiotic intervention trials, these scores combined with baseline bacterial abundance predicted post-treatment persistence in roughly 69% of trial-probiotic pairs.
That's a meaningful finding, and it reframes the whole question. The issue isn't just "do probiotics work?" It's "does this probiotic work in this person's gut?" Those are very different questions, and the second one is currently unanswerable at the pharmacy counter.
Mayo Clinic's guidance draws a useful distinction here: probiotics add live microbes directly, while prebiotics — dietary fiber that feeds microbes already present — nourish what's already there. For most healthy people, the evidence for prebiotics (i.e., eating more plants and fiber) is considerably more consistent than the evidence for probiotic supplements.
What to Actually Do With This
A few things hold up under scrutiny. Probiotic evidence is strongest for specific clinical contexts — certain strains for antibiotic-associated diarrhea, for instance — rather than general "gut health." If you have a specific condition, it's worth asking a gastroenterologist about strain-specific evidence, not just grabbing whatever's on sale.
For the general population, the honest answer is: we don't yet know whose microbiome will respond to which strains, and no product currently on the market can tell you. The Nature Communications research points toward a future where that personalization might be possible — but that future isn't the probiotic aisle in 2026.
The most evidence-backed thing you can do for your gut microbiome remains deeply unsexy: eat a varied diet high in fiber, minimize unnecessary antibiotics, and don't smoke. Probiotics might help some people some of the time. They probably won't hurt. But "probably harmless" is a long way from the confident promise on the label.