Somewhere along the way, "breakfast is the most important meal of the day" became one of those facts that feels too obvious to question. It's on cereal boxes, in school nutrition pamphlets, in the advice of every well-meaning parent who ever pushed eggs across a kitchen table. The claim is so embedded in health culture that most people have never stopped to ask where it came from — or whether it holds up.
The short answer: the origin is mostly marketing, the evidence is genuinely mixed, and the more interesting question turns out to be not whether you eat breakfast but when you eat anything at all.
The Claim: First Meal, Best Meal
The popular belief goes something like this: eating breakfast jumpstarts your metabolism, stabilizes blood sugar, improves concentration, and sets you up for better food choices throughout the day. Skip it, and you're inviting weight gain, energy crashes, and metabolic trouble.
This framing has been remarkably durable. It survived the low-fat era, the low-carb era, and the intermittent fasting boom — though that last one put some real pressure on it. The breakfast-as-essential narrative is so culturally ingrained that even people who skip breakfast regularly often describe it as a guilty habit rather than a deliberate choice.
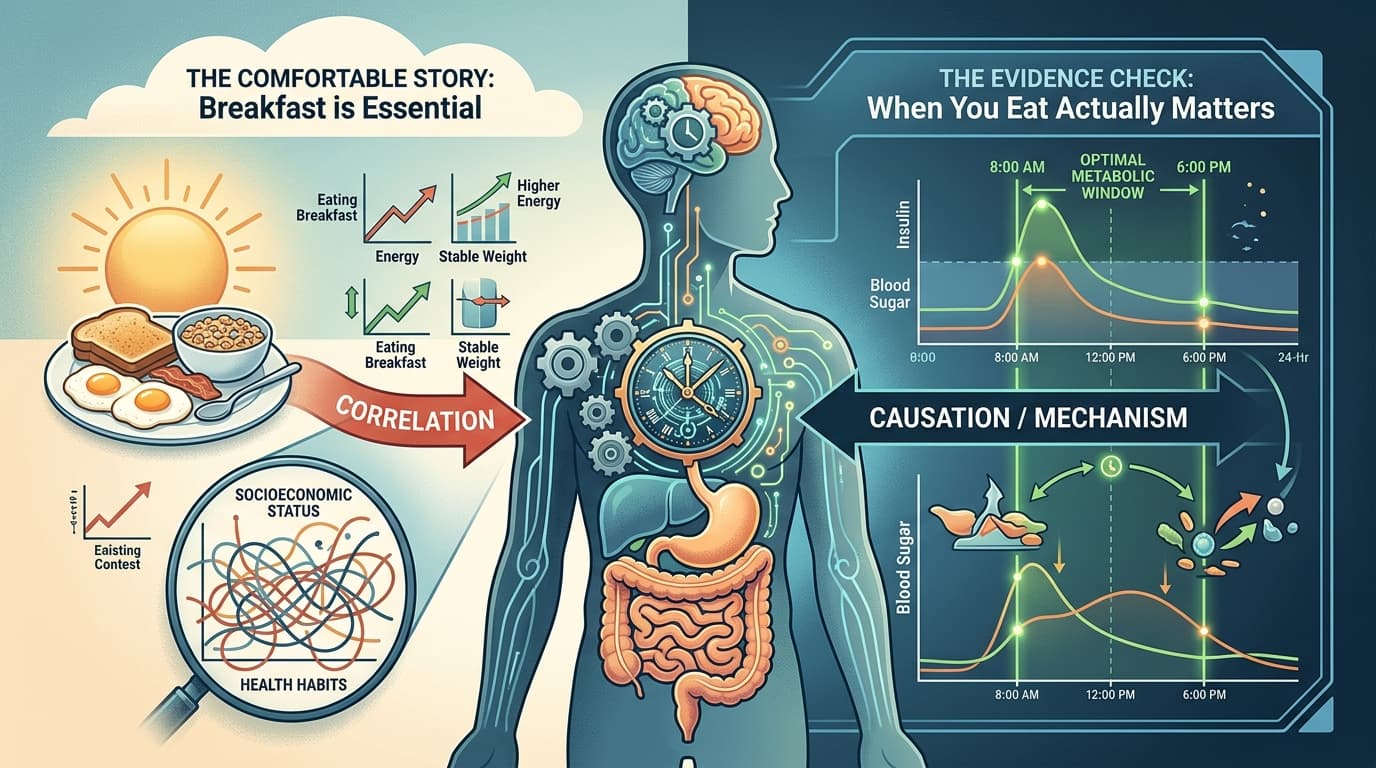
Why the Belief Sticks: Correlation Is a Comfortable Story
Part of the appeal is that the observational data looks convincing at first glance. Studies consistently show that people who eat breakfast tend to have lower rates of obesity, better metabolic markers, and healthier overall diets. If you're not reading carefully, that sounds like evidence that breakfast causes those outcomes.
It doesn't. People who eat breakfast regularly also tend to have more structured routines, higher incomes, better sleep, and more stable food environments. Disentangling breakfast itself from that cluster of behaviors is genuinely hard, and most of the studies that built the "breakfast is essential" consensus didn't try very hard to do it.
There's also a psychological dimension worth naming: breakfast feels virtuous. It signals discipline, planning, and self-care. Skipping it feels like cutting corners. That moral weight makes the claim stickier than the evidence warrants.
What the Research Actually Shows: Timing Over Timing
The honest summary of the current evidence is that breakfast per se — the first meal of the day, eaten in the morning — doesn't have the metabolic significance its reputation suggests. What does appear to matter is the overall pattern of when you eat across the day, and specifically how that pattern aligns with your body's circadian rhythms.
A cross-sectional study published in Frontiers in Nutrition examining adults aged 35–74 found that skipping breakfast was associated with increased risk of metabolic syndrome, but the authors were careful to note that evidence remains limited and that cross-sectional designs can't establish causation. That's an important caveat the headline version of this research tends to drop.
Meanwhile, the time-restricted eating literature has been quietly reshaping how researchers think about meal timing altogether. A recent review in Current Nutrition Reports summarizing randomized controlled trials found that time-restricted eating — compressing food intake into a defined window — shows meaningful effects on body weight and cardiometabolic risk factors in people with obesity. The mechanism isn't about breakfast specifically; it's about aligning eating with metabolic readiness and avoiding late-night intake.
That last part is where things get genuinely interesting. A large analysis of 14,012 adults from NHANES data found that earlier last meals — specifically before 9 p.m. — were linked to better biological aging markers across multiple organs, including the heart, liver, and kidneys. The signal wasn't about when people started eating. It was about when they stopped.
A separate study on time-restricted eating in adults with overweight, obesity, and type 2 diabetes found that TRE induces a metabolic shift toward increased lipolysis and ketogenesis — changes that affect energy balance in ways that go well beyond simple calorie restriction. Again, the mechanism is about the eating window and its relationship to metabolic cycles, not about the morning meal as a special category.
The emerging field of chrononutrition — which examines how eating patterns interact with biological rhythms — frames meal timing as a meaningful variable in its own right, distinct from meal composition or frequency. That's a genuinely different frame than "eat breakfast, skip breakfast." It asks: when is your body actually prepared to process food efficiently, and are you eating in sync with that or against it?
The honest answer is that we don't have clean, definitive answers yet. Most time-restricted eating trials are relatively short, sample sizes vary considerably, and individual responses to meal timing differ based on chronotype, sleep patterns, and metabolic health status. The research is promising but not settled.
What to Actually Take From This
A few things seem reasonably solid, with appropriate uncertainty attached:
The breakfast mandate is oversold. If you're not hungry in the morning, forcing yourself to eat because of a decades-old nutritional axiom isn't well-supported by current evidence. Hunger cues and individual variation matter.
When you stop eating may matter more than when you start. The consistent signal across multiple lines of research points toward late-night eating as a meaningful metabolic stressor. If you're going to make one timing change, finishing dinner earlier is better supported than forcing breakfast earlier.
Eating window consistency probably matters. The time-restricted eating literature suggests that compressing your eating into a defined, consistent window — whatever that window is — has cardiometabolic benefits, particularly for people with obesity or metabolic dysfunction. The specific hours matter less than the regularity.
Context is everything. Children, athletes, people with diabetes, shift workers, and people recovering from illness all have different relationships with meal timing. "Breakfast is important" might be genuinely true for a ten-year-old with a full school day ahead and less true for an adult with a flexible morning schedule and no appetite until noon.
The breakfast myth persists because it's simple, it sounds responsible, and it was marketed aggressively for a long time. The actual biology is more interesting and considerably more complicated. Your circadian rhythm doesn't care whether you call the first meal of the day breakfast — it cares whether you're eating at 10 p.m. when your liver would rather be doing something else.